(406) Synergistic Impact of Donor KIR-BX Haplotypes and Recipient HLA-C1 Homozygosity on Survival Outcomes in Pediatric Haploidentical Hematopoietic Cell Transplantation: A Retrospective Cohort Study of 153 Cases

Xiangjun Liu, PhD (he/him/his)
– CEO, BFR Gene Diagnostics, China (People's Republic)
Speaker(s)
Aim: Donor KIR-B/X haplotypes have demonstrated survival benefits in adult AML patients undergoing unrelated hematopoietic cell transplantation (HCT), particularly in HLA-C1-positive recipients (PMID:35238913). This KIR-HLA interaction was further explored in cord blood transplantation cohorts showing reduced relapse-related mortality (PMID:37206286). Recent evidence suggests that in anti-thymocyte globulin (ATG)-based haploidentical HCT, the enhanced activating KIR (aKIR) profile of B/X haplotypes may potentiate NK cell cytotoxicity, improving outcomes in adult AML (PMID:36761162). However, the pediatric-specific interplay between donor KIR haplotypes (AA vs B/X) and recipient HLA-C polymorphisms remains uncharacterized.
Methods: We analyzed 153 consecutive pediatric patients (82 AML, 60 ALL, 7 MPAL, 4 other malignancies) undergoing ATG-based haplo-HCT between 2017-2023 at Beijing Children's Hospital. Recipients were stratified by HLA-C status (C1/C1 vs C2+), with KIR genotyping performed for all donors. Clinical endpoints included OS, DFS, relapse, and NRM. Survival analyses employed Kaplan-Meier method with log-rank test, while competing risks were assessed using Gray's test. Multivariable Cox regression models adjusted for disease type and age.
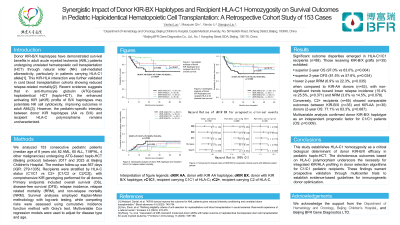
Results: Significant outcome disparities emerged in HLA-C1/C1 recipients (n=88). Those receiving KIR-B/X grafts (n=35) exhibited superior 2-year OS (97.0% vs 63.0%, p=0.004) and DFS (81.5% vs 57.6%, p=0.034) compared to KIR-AA donors (n=53), with non-significant trends toward lower relapse (15.4% vs 25.5%, p=0.371) and NRM (3.0% vs 14.5%, p=0.078). Conversely, C2+ recipients (n=65) showed comparable outcomes between KIR-B/X (n=35) and KIR-AA (n=30) donors (2-year OS: 77.1% vs 83.3%, p=0.687). Multivariable analysis confirmed donor KIR-B/X haplotype as an independent prognostic factor for C1/C1 patients (OS: p=0.009).
Conclusion: This study establishes HLA-C1 homozygosity as a critical biological determinant of donor KIR-B/X efficacy in pediatric ATG-based haplo-HCT, which underscores the necessity for integrated KIR/HLA profiling in donor selection algorithms for C1/C1 pediatric recipients. These findings warrant prospective validation through multicenter trials to establish evidence-based guidelines for immunogenetic donor optimization.
Methods: We analyzed 153 consecutive pediatric patients (82 AML, 60 ALL, 7 MPAL, 4 other malignancies) undergoing ATG-based haplo-HCT between 2017-2023 at Beijing Children's Hospital. Recipients were stratified by HLA-C status (C1/C1 vs C2+), with KIR genotyping performed for all donors. Clinical endpoints included OS, DFS, relapse, and NRM. Survival analyses employed Kaplan-Meier method with log-rank test, while competing risks were assessed using Gray's test. Multivariable Cox regression models adjusted for disease type and age.
Results: Significant outcome disparities emerged in HLA-C1/C1 recipients (n=88). Those receiving KIR-B/X grafts (n=35) exhibited superior 2-year OS (97.0% vs 63.0%, p=0.004) and DFS (81.5% vs 57.6%, p=0.034) compared to KIR-AA donors (n=53), with non-significant trends toward lower relapse (15.4% vs 25.5%, p=0.371) and NRM (3.0% vs 14.5%, p=0.078). Conversely, C2+ recipients (n=65) showed comparable outcomes between KIR-B/X (n=35) and KIR-AA (n=30) donors (2-year OS: 77.1% vs 83.3%, p=0.687). Multivariable analysis confirmed donor KIR-B/X haplotype as an independent prognostic factor for C1/C1 patients (OS: p=0.009).
Conclusion: This study establishes HLA-C1 homozygosity as a critical biological determinant of donor KIR-B/X efficacy in pediatric ATG-based haplo-HCT, which underscores the necessity for integrated KIR/HLA profiling in donor selection algorithms for C1/C1 pediatric recipients. These findings warrant prospective validation through multicenter trials to establish evidence-based guidelines for immunogenetic donor optimization.
