(323) SARS-CoV2 Infection Post-transplantation Induces Transient HLA Antibodies in Pediatric Heart Recipients
.jpg)
Phillip Erice, PhD
– Postdoctoral associate, Baylor College of Medicine
Speaker(s)
Aim: Heart transplant (HTx) recipients with donor-specific HLA antibodies (DSA) experience lowered freedom from cardiac allograft vasculopathy, increased risk for chronic rejection, and decreased graft survival. Post-HTx recipients are placed on an immunosuppressive regimen that mitigates the production of HLA antibodies but paradoxically increases the risk of infection which can act as an immunogenic stimulus of said antibodies. Here we report a retrospective longitudinal study to examine the post-transplant formation and persistence of anti-HLA antibodies, including DSA, following SARS-CoV2 infection in a cohort of pediatric HTx patients.
Methods: We reviewed 31 pediatric HTx recipients who tested positive for SARS-CoV2 following transplantation. HLA antibodies were assessed by flow PRA bead and SAB assays in serum prior to testing positive for SARS-CoV2 and at 6 months-,1 year-, and 3 years-post the initial SARS-CoV2 positive test date [denoted SARS-CoV2(+)].
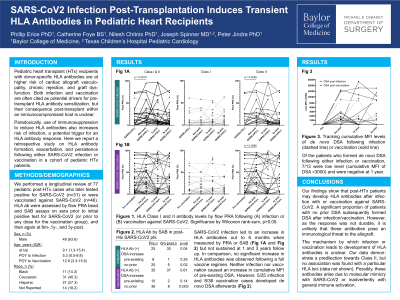
Results: Post-transplant HLA antibodies identified by flow PRA were increased at 6 months following SARS-CoV2(+) but not from serial sampling at 1 or 3 years (Figure 1). Parallel assessment of HLA antibodies by SAB were also significantly increased (p=0.04) post-SARS-CoV2(+) but did not reveal any predilection towards a particular HLA locus or antigen. Of the 31 cases, 6 had post-HTx DSA prior to infection, but only 1 of those patients saw an increase in the cumulative sum MFI of their DSA (Figure 2). Whereas 25 patients had no post-HTx DSA prior to infection, of which 5 developed DSA following SARS-CoV2(+) (p=0.002).
Conclusion: Our findings show that post-HTx patients under immunosuppression can develop HLA antibodies after SARS-CoV2 infection. As the response is not durable, it is unclear whether these antibodies pose an immunological threat to the allograft. However, of the patients who had no DSA prior to infection, a significant proportion subsequently developed DSA after testing positive for SARS-CoV2. Similar to the general HLA antibody response following SARS-CoV2 infection, in four of those five cases, DSA remained low-level or eventually resolved over time.
Methods: We reviewed 31 pediatric HTx recipients who tested positive for SARS-CoV2 following transplantation. HLA antibodies were assessed by flow PRA bead and SAB assays in serum prior to testing positive for SARS-CoV2 and at 6 months-,1 year-, and 3 years-post the initial SARS-CoV2 positive test date [denoted SARS-CoV2(+)].
Results: Post-transplant HLA antibodies identified by flow PRA were increased at 6 months following SARS-CoV2(+) but not from serial sampling at 1 or 3 years (Figure 1). Parallel assessment of HLA antibodies by SAB were also significantly increased (p=0.04) post-SARS-CoV2(+) but did not reveal any predilection towards a particular HLA locus or antigen. Of the 31 cases, 6 had post-HTx DSA prior to infection, but only 1 of those patients saw an increase in the cumulative sum MFI of their DSA (Figure 2). Whereas 25 patients had no post-HTx DSA prior to infection, of which 5 developed DSA following SARS-CoV2(+) (p=0.002).
Conclusion: Our findings show that post-HTx patients under immunosuppression can develop HLA antibodies after SARS-CoV2 infection. As the response is not durable, it is unclear whether these antibodies pose an immunological threat to the allograft. However, of the patients who had no DSA prior to infection, a significant proportion subsequently developed DSA after testing positive for SARS-CoV2. Similar to the general HLA antibody response following SARS-CoV2 infection, in four of those five cases, DSA remained low-level or eventually resolved over time.
