(322) Donor-Recipient Age Difference as a Predictor of eGFR in HLA-A, HLA-B, HLA-DR Mismatch Renal Transplant Recipients in a Tertiary Care Teaching Hospital

Shubhi Shrivastava
– Final Year MBBS Student, Mahatma Gandhi Medical College & Hospital, Jaipur, India, India
Speaker(s)
Aim: To determine the association between donor-recipient age difference and eGFR in HLA-A, HLA-B and HLA-DR mismatch renal transplant recipients.
Methods: This retrospective case-control study was conducted at a tertiary care teaching hospital in North-West India. Medical records of patients diagnosed with End-Stage Renal Disease who underwent kidney transplantation between March 2019 and August 2024 were reviewed. Relevant clinical and laboratory parameters were systematically extracted and compiled into a Microsoft Excel database for subsequent statistical analysis.
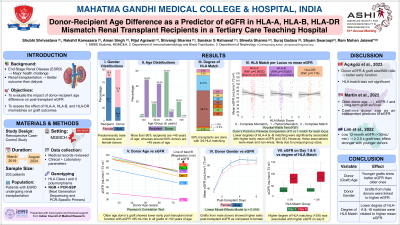
Results: A total of 203 transplant recipients contributed 1,218 eGFR observations from post-operative days 1 through 6. The mean age of kidney transplant recipients was 31.7 years, and that of donors was 52.8 years. Recipients with HLA-A matching had a higher mean age (31.8 vs. 24.0 years) compared to those with A-mismatch, and their donors were also older (52.9 vs. 49.7 years). In contrast, no significant age differences were observed between matched and mismatched groups for HLA-B (recipient: 31.6 vs. 31.9 years; donor: 52.5 vs. 53.4 years) or HLA-DR (recipient: 31.6 vs. 32.2 years; donor: 52.6 vs. 53.1 years). This suggests that HLA-A mismatches are more common in younger donor-recipient pairs.
A linear mixed-effects model using Restricted Maximum Likelihood showed that older donor age (β = −0.23, p = 0.025) and recipient age (β = −0.56, p = 0.004) were linked to lower eGFR. Kidneys from male donors were linked to higher eGFR (β = 4.78, p = 0.016).
Conclusion: The data demonstrate the direct effect of donor age on early post-transplant eGFR and long-term allograft survival. In particular, graft survival is lower with increasing donor age, which is independent of the degree of HLA mismatch. HLA mismatching is still a major risk factor for graft loss, but this can have a less negative impact by choosing a younger donor and hence increasing the chance of a successful transplant while minimising risk of graft loss.
Methods: This retrospective case-control study was conducted at a tertiary care teaching hospital in North-West India. Medical records of patients diagnosed with End-Stage Renal Disease who underwent kidney transplantation between March 2019 and August 2024 were reviewed. Relevant clinical and laboratory parameters were systematically extracted and compiled into a Microsoft Excel database for subsequent statistical analysis.
Results: A total of 203 transplant recipients contributed 1,218 eGFR observations from post-operative days 1 through 6. The mean age of kidney transplant recipients was 31.7 years, and that of donors was 52.8 years. Recipients with HLA-A matching had a higher mean age (31.8 vs. 24.0 years) compared to those with A-mismatch, and their donors were also older (52.9 vs. 49.7 years). In contrast, no significant age differences were observed between matched and mismatched groups for HLA-B (recipient: 31.6 vs. 31.9 years; donor: 52.5 vs. 53.4 years) or HLA-DR (recipient: 31.6 vs. 32.2 years; donor: 52.6 vs. 53.1 years). This suggests that HLA-A mismatches are more common in younger donor-recipient pairs.
A linear mixed-effects model using Restricted Maximum Likelihood showed that older donor age (β = −0.23, p = 0.025) and recipient age (β = −0.56, p = 0.004) were linked to lower eGFR. Kidneys from male donors were linked to higher eGFR (β = 4.78, p = 0.016).
Conclusion: The data demonstrate the direct effect of donor age on early post-transplant eGFR and long-term allograft survival. In particular, graft survival is lower with increasing donor age, which is independent of the degree of HLA mismatch. HLA mismatching is still a major risk factor for graft loss, but this can have a less negative impact by choosing a younger donor and hence increasing the chance of a successful transplant while minimising risk of graft loss.
