(320) Assessing the Impact of Induction Regimen on Graft Function in HLA-A, HLA-B, HLA- DR Mismatch Renal Transplant: A Retrospective Study

Shubhi Shrivastava
– Final Year MBBS Student, Mahatma Gandhi Medical College & Hospital, Jaipur, India, India
Speaker(s)
Aim: To identify any association between the efficacy of drug used induction regimen and short term graft function (eGFR) in HLA-A, HLA-B, HLA- DR mismatch renal transplant patients.
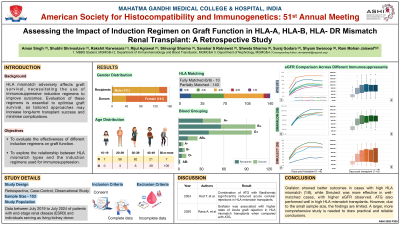
Methods: This retrospective, case-control epidemiological study was conducted at a tertiary care teaching facility in Northwest India. The study population included patients suffering from end-stage renal disease (ESRD) who had undergone renal transplantation. Data for this study was collected from existing written medical records of ESRD patients and healthy kidney donors. Patients and donors with missing data were excluded. Data from April 2019 to July 2024 was analysed, resulting in a sample size of 153 patients. To estimate post-transplant renal function, eGFR was evaluated for the first six days following transplantation.
Results: A linear mixed-effects model was used to evaluate the association between HLA mismatches (A, B, DR loci) and induction immunosuppressive therapies (ATG, grafalon, simulect) on estimated glomerular filtration rate (eGFR). Compared to ATG, grafalon was associated with significantly higher eGFR values (β = 35.75, p = 0.028), while simulect showed a borderline effect (β = 25.88, p = 0.051) in cases of no HLA mismatch. Simulect has strong borderline effect (–25.34, p = 0.052) on eGFR in Mismatch HLA-B patients.
Conclusion: Our study found that the use of an induction regimen can have varied effects on graft function in HLA mismatched patients, therefore the induction regimen must be chosen with caution. In conclusion the drug simulect was found to be more closely associated with better short term graft function in no mismatch transplants while decreased short term graft function in HLA-B mismatch patients was observed. Also, donor age was negatively associated with graft function in the first half of the observation period.
Methods: This retrospective, case-control epidemiological study was conducted at a tertiary care teaching facility in Northwest India. The study population included patients suffering from end-stage renal disease (ESRD) who had undergone renal transplantation. Data for this study was collected from existing written medical records of ESRD patients and healthy kidney donors. Patients and donors with missing data were excluded. Data from April 2019 to July 2024 was analysed, resulting in a sample size of 153 patients. To estimate post-transplant renal function, eGFR was evaluated for the first six days following transplantation.
Results: A linear mixed-effects model was used to evaluate the association between HLA mismatches (A, B, DR loci) and induction immunosuppressive therapies (ATG, grafalon, simulect) on estimated glomerular filtration rate (eGFR). Compared to ATG, grafalon was associated with significantly higher eGFR values (β = 35.75, p = 0.028), while simulect showed a borderline effect (β = 25.88, p = 0.051) in cases of no HLA mismatch. Simulect has strong borderline effect (–25.34, p = 0.052) on eGFR in Mismatch HLA-B patients.
Conclusion: Our study found that the use of an induction regimen can have varied effects on graft function in HLA mismatched patients, therefore the induction regimen must be chosen with caution. In conclusion the drug simulect was found to be more closely associated with better short term graft function in no mismatch transplants while decreased short term graft function in HLA-B mismatch patients was observed. Also, donor age was negatively associated with graft function in the first half of the observation period.
