(222) Mycophenolate Mofetil Dosing Impacts Humoral and Cellular Responses to SARS-CoV-2 in Patients Hospitalized with COVID-19

Harry Pickering, PhD
– Assistant Professor, UCLA, United States
Speaker(s)
Aim: COVID-19 poses significant risks for solid organ transplant (SOT) recipients, who have atypical immune responses to SARS-CoV-2, with mycophenolate mofetil (MMF) immunotherapy potentially further diminishing responsiveness. We sought to understand the impact of MMF and its dosing on early immune responses in hospitalized patients.
Methods: We studied 27 SOT recipients and 56 non-SOT controls from UCLA enrolled in the multicenter IMPACC study at days 1-3 post-admission. SOT recipients were grouped based on MMF dosing at admission into ≤1000 mg/day or >1000 mg/day. Anti-RBD and spike IgG levels were measured in serum. Peripheral blood mononuclear cells were stimulated with a SARS-CoV-2 spike-specific peptide pool and memory T cells were profiled by flow cytometry for activation-induced markers and cytokine production.
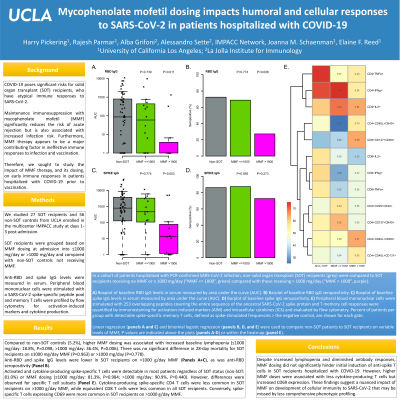
Results: Compared to non-SOT controls (5.2%), higher MMF dosing was associated with increased baseline lymphopenia (≤1000 mg/day: 18.8%, P=0.098; >1000 mg/day: 36.4%, P=0.006). There was no significant difference in 28-day mortality for SOT recipients on ≤1000 mg/day MMF (P=0.963) or >1000 mg/day (P=0.778). Anti-RBD and spike IgG levels were lower in SOT recipients on >1000 g/day MMF (Fig. 1A+C), as was anti-RBD seropositivity (Fig. 1B). Activated and cytokine-producing spike-specific T cells were detectable in most patients regardless of SOT status (non-SOT: 81.0%) or MMF dosing (≤1000 mg/day: 81.3%, P=0.984; >1000 mg/day: 90.9%, P=0.440). However, differences were observed for specific T cell subsets (Fig. 1E). Cytokine-producing spike-specific CD4 T cells were less common in SOT recipients on >1000 g/day MMF, while equivalent CD8 T cells were less common in all SOT recipients. Conversely, spike-specific T cells expressing CD69 were more common in SOT recipients on >1000 g/day MMF.
Conclusion: Despite increased lymphopenia and diminished antibody responses, MMF dosing did not significantly hinder initial induction of anti-spike T cells in SOT recipients hospitalized with COVID-19. However, higher MMF doses were associated with less cytokine-producing T cells but increased CD69 expression. These findings suggest a nuanced impact of MMF on development of cellular immunity to SARS-CoV-2 that may be missed by less comprehensive phenotypic profiling.
Methods: We studied 27 SOT recipients and 56 non-SOT controls from UCLA enrolled in the multicenter IMPACC study at days 1-3 post-admission. SOT recipients were grouped based on MMF dosing at admission into ≤1000 mg/day or >1000 mg/day. Anti-RBD and spike IgG levels were measured in serum. Peripheral blood mononuclear cells were stimulated with a SARS-CoV-2 spike-specific peptide pool and memory T cells were profiled by flow cytometry for activation-induced markers and cytokine production.
Results: Compared to non-SOT controls (5.2%), higher MMF dosing was associated with increased baseline lymphopenia (≤1000 mg/day: 18.8%, P=0.098; >1000 mg/day: 36.4%, P=0.006). There was no significant difference in 28-day mortality for SOT recipients on ≤1000 mg/day MMF (P=0.963) or >1000 mg/day (P=0.778). Anti-RBD and spike IgG levels were lower in SOT recipients on >1000 g/day MMF (Fig. 1A+C), as was anti-RBD seropositivity (Fig. 1B). Activated and cytokine-producing spike-specific T cells were detectable in most patients regardless of SOT status (non-SOT: 81.0%) or MMF dosing (≤1000 mg/day: 81.3%, P=0.984; >1000 mg/day: 90.9%, P=0.440). However, differences were observed for specific T cell subsets (Fig. 1E). Cytokine-producing spike-specific CD4 T cells were less common in SOT recipients on >1000 g/day MMF, while equivalent CD8 T cells were less common in all SOT recipients. Conversely, spike-specific T cells expressing CD69 were more common in SOT recipients on >1000 g/day MMF.
Conclusion: Despite increased lymphopenia and diminished antibody responses, MMF dosing did not significantly hinder initial induction of anti-spike T cells in SOT recipients hospitalized with COVID-19. However, higher MMF doses were associated with less cytokine-producing T cells but increased CD69 expression. These findings suggest a nuanced impact of MMF on development of cellular immunity to SARS-CoV-2 that may be missed by less comprehensive phenotypic profiling.
