(205) Specific HLA-DQ G1/G2 Mismatches Affect Myeloid Malignancy Relapse Incidence in Haploidentical HCT

Ping Rao, PhD
– Associate Director, City of Hope, United States
Speaker(s)
Aim: HLA-DQ G1 heterodimers comprise DQ2/3/4 antigens which have many peptide residues not found in G2 heterodimers (DQ5, DQ6). HLA-DQ has been indicated as particularly important to de novo antibody development and patient G2 heterodimer genotype content has been linked to relapse in studies of haploidentical and unrelated donors. We sought to determine if the HLA-DQ G1/G2 genotype of patients and donors affected relapse or other outcomes in publicly available CIBMTR data of haploidentical HCT cases.
Methods: We conducted a retrospective analysis using the publicly available P-5545 dataset of patients with haploidentical transplant with post-transplant cyclophosphamide from the Center for International Blood and Marrow Transplant Research (CIBMTR), available at https://cibmtr.org. The data set contained eplet analysis information performed by the original study authors. Data was analyzed with R v3.6.3 using survival, cmprsk, and survminer packages.
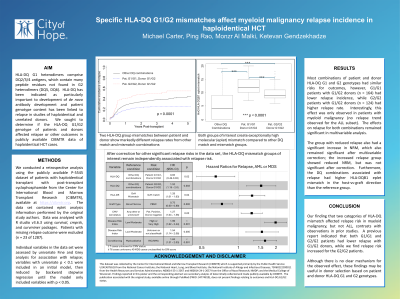
Results: Most combinations of patient and donor HLA-DQ G1 and G2 genotypes had similar risks for outcomes, however, G1/G1 patients with G1/G2 donors had lower relapse incidence, while G2/G2 patients with G1/G2 donors had higher relapse rate. Interestingly, this effect was only observed in patients with myeloid malignancy (no relapse trend observed for the ALL subset). The effects on relapse for both combinations remained significant in multivariable analysis. The group with reduced relapse also had a significant increase in NRM, which also remained significant after multivariable correction; the increased relapse group showed reduced NRM, but was not significant after correction. Furthermore, the DQ combinations associated with relapse had higher HLA-DQB1 eplet mismatch in the host-vs-graft direction than the reference group.
Conclusion: Our finding that two categories of HLA-DQ mismatch affected relapse risk in myeloid malignancy, but not ALL, contrasts with observations in prior studies. A previous report indicated that both G1/G1 and G2/G2 patients had lower relapse with G1/G2 donors, while we find relapse risk increased for the G2/G2 patients. Although there is no clear mechanism for the observed effect, these findings may be useful in donor selection based on patient and donor HLA-DQ G1 and G2 genotypes.
Footnotes: This dataset was collected by the Center for International Blood and Marrow Transplant Research (CIBMTR) which is supported primarily by the Public Health Service U24CA076518 from the National Cancer Institute; the National Heart, Lung, and Blood Institute; the National Institute of Allergy and Infectious Diseases; 75R60222C00011 from the Health Resources and Services Administration; N00014-23-1-2057 and N00014-24-1-2057 from the Office of Naval Research; NMDP; and the Medical College of Wisconsin. Findings reported in this abstract are secondary analysis of data initially collected and made publicly available by CIBMTR. The publication associated with the original study, available online through PubMed (PMID: 34774819), does not present findings relating to outcomes and HLA-DQ G1/G2 status.
Methods: We conducted a retrospective analysis using the publicly available P-5545 dataset of patients with haploidentical transplant with post-transplant cyclophosphamide from the Center for International Blood and Marrow Transplant Research (CIBMTR), available at https://cibmtr.org. The data set contained eplet analysis information performed by the original study authors. Data was analyzed with R v3.6.3 using survival, cmprsk, and survminer packages.
Results: Most combinations of patient and donor HLA-DQ G1 and G2 genotypes had similar risks for outcomes, however, G1/G1 patients with G1/G2 donors had lower relapse incidence, while G2/G2 patients with G1/G2 donors had higher relapse rate. Interestingly, this effect was only observed in patients with myeloid malignancy (no relapse trend observed for the ALL subset). The effects on relapse for both combinations remained significant in multivariable analysis. The group with reduced relapse also had a significant increase in NRM, which also remained significant after multivariable correction; the increased relapse group showed reduced NRM, but was not significant after correction. Furthermore, the DQ combinations associated with relapse had higher HLA-DQB1 eplet mismatch in the host-vs-graft direction than the reference group.
Conclusion: Our finding that two categories of HLA-DQ mismatch affected relapse risk in myeloid malignancy, but not ALL, contrasts with observations in prior studies. A previous report indicated that both G1/G1 and G2/G2 patients had lower relapse with G1/G2 donors, while we find relapse risk increased for the G2/G2 patients. Although there is no clear mechanism for the observed effect, these findings may be useful in donor selection based on patient and donor HLA-DQ G1 and G2 genotypes.
Footnotes: This dataset was collected by the Center for International Blood and Marrow Transplant Research (CIBMTR) which is supported primarily by the Public Health Service U24CA076518 from the National Cancer Institute; the National Heart, Lung, and Blood Institute; the National Institute of Allergy and Infectious Diseases; 75R60222C00011 from the Health Resources and Services Administration; N00014-23-1-2057 and N00014-24-1-2057 from the Office of Naval Research; NMDP; and the Medical College of Wisconsin. Findings reported in this abstract are secondary analysis of data initially collected and made publicly available by CIBMTR. The publication associated with the original study, available online through PubMed (PMID: 34774819), does not present findings relating to outcomes and HLA-DQ G1/G2 status.
